Ankle disease usually presents with pain and swelling in the ankle joint line. The joint is painful to move. Although the ligaments are eroded the ankle is not usually unstable. Some patients with severe erosion of the ankle may also have hindfoot valgus, although this is usually due to a combination of abnormal limb biomechanics, subtalar/talonavicular erosion and tibialis posterior tendonopathy (see below). The proximal limb joints, overall limb alignment and the forefoot should also be assessed.
It is not always easy to distinguish between pain arising in the ankle or the hindfoot joints, but this distinction may determine the extent of surgery that is required. Clinical examination, plain radiography, ultrasound or MRI, and diagnostic injections may help.
Plain radiographs will demonstrate joint damage, erosions and periarticular osteopenia – standing AP/lateral are standard views. MRI or ultrasound may demonstrate synovitis or erosions that are not seen on plain radiography. If there is hindfoot valgus a standing hindfoot alignment view (Saltzmann and el-Khoury 1994) helps to define the contributions of ankle and subtalar tilt.
Non-surgical treatment
Steroid injections are often helpful on an empirical basis, although there is no good evidence base for their use and in other joints they may not be much better than placebo. Rest/immobilisation and custom orthotics/bracing are often beneficial. An AFO might be required to improve alignment of the ankle and hindfoot.
Surgery
Synovectomy
A long-term Japanese study reported recurrent disease in only 10% of ankles at 10-20 year follow-up of open synovectomy (Akagi et al 1997). Synovectomy is beneficial in 80% across all joints, mainly elbows and knees (Chalmers 2011); about half showed radiographic progression and this was commoner after arthroscopic than open procedures. Van der Zant reported good improvement in 56% of patients who underwent rhenium-186 synovial ablation, with a median duration of action of 41months; however, disease recurred in all patients by 75m. Liepe (2011) reported a good response at 3 months in 64% but no long term follow-up.
Ankle fusion
Fusion is the traditional treatment for end-stage ankle arthritis, and remains a viable option. Arthroscopic fusion results in quicker and more reliable fusion, with fewer soft-tissue complications than open fusion, and should be viewed as the standard technique unless there is severe deformity, bone loss or infection.
Over 15 series of arthroscopic ankle fusions have been reported. The largest series is that of Winson (2005). 118 fusions were reported, of which 105 were followed clinically for a mean of 65m. 109/118 procedures fused at a mean of 12weeks. Most non-unions happened early in the series, and subsequently the authors immobilised all patients for a minimum of 12 weeks. Smoking was twice as common in non-unions. There were three superficial and one deep infection, one malunion and two pulmonary emboli. Winson recommended arthroscopic fusion even if the ankle was in valgus or varus provided the forefoot was plantigrade.
Gougiolias (2007), however, carried out arthroscopic fusions even if there was mortise deformity and the foot was not plantigrade, by excising bone from the mortise arthroscopically to align the ankle. 30/78 patients had a pre-operative coronal deformity of >15deg, but none had more than 3deg post-operatively. Five patients had simultaneous arthroscopic subtalar fusion. There were 5 delayed unions and 2 non-unions; time to union was 2months extra in smokers. There was one PE, one nerve injury and 6 patients had subtalar pain.
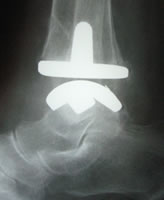
Mobility ankle replacement
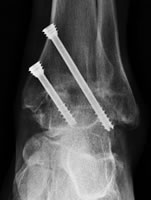
Arthroscopic ankle fusion
Many surgeons favour ankle replacement over fusion in inflammatory arthritis to maximise function and reduce stresses on other at-risk joints. However, the available evidence suggests little difference between overall results.
Overall about 550 arthroscopic fusions have been reported with a total fusion rate of 93.3%. Several series have commented on the quicker rate of union in arthroscopic procedures although this can be influenced by the intervals at which radiographs are taken, and all series diagnosed union on plain radiography rather than CT. Myerson (1996) noted a mean time of fusion of 8.7 weeks in arthroscopic versus 14.5 weeks in open fusions, while Nielsen (2008) noted that 90% of arthroscopic and 57% of open fusions were united at 12 weeks. However, there are relatively few rheumatoid patients in these series.
Open fusion may be done using anterior, lateral or posterior approaches. Maenpaa reported a 90% failure rate in 130 rheumatoid patients, while Felix et al (1998) reported union in 96% of 26 ankles at 2-8 year follow-up, and no pain.
Ankle replacement
Second-generation prostheses from the late 1980s onward introduced improved engineering, often with three components. 10-20 year results are now being published (Kofoed 2004, Buechel et al 2004), indicating success in over 90% of patients. However, these are the series of the designers of the various prostheses, and further results from the “real world” may not be quite so optimistic. The Wrightington series (Wood 2003, 2008) is a realistic and critical account with 92% survival at 5 year and 80% at 10 years. The Swedish register reported 70% 10-year survival and the Norwegian registry 76% 10-year survival. In all these series the survival was the same in RA and OA; Wood reported a higher rate of soft tissue complications in RA. Hindfoot deformity may need to be corrected separately or at the same procedure (Kim 2010).
Fusion versus replacement in the rheumatoid patient
As might be expected, ankle fusion affects the range of motion and kinematics more than does replacement, and certain designs are closer to normal than others (Valderrabano et al 2004a,b). Gait analysis is much closer to normal in replaced than in fused ankles (Butcher 2004, Piriou 2008). Hence it is plausible that ankle replacements would place less stress on other joints, both in the tarsus and proximally. Nevertheless, this requires clinical confirmation.
There are, remarkably, no RCTs comparing replacement with fusion, and only one prospective comparative trial, which excluded patients with inflammatory disease (Saltzman 2009, 2010). At 4 years, this study reported better function in the replacements, with equal pain improvement in both groups. A systematic review of the literature by Haddad et al (2007) found the overall reported results of both procedures to be similar, with about 70% satisfactory results after both procedures. The overall non-union rate for ankle fusion was 10% and the arthroplasty survival rate 77% at 10 years. There was more variation in results for arthroplasty. Younger (2010) also found similar overall results for fusion and replacement. SooHoo (2007) and Younger (2011) reported more adverse events after replacement, but SooHoo also reported more subtalar fusions after fusion. None of these series differentiated between RA and OA.
Many surgeons tend to favour ankle replacement for patients with polyarthritis with a view to maximizing retained function and minimizing the risk of adjacent arthritis. While this is not based on strong evidence, it is clinically plausible.
© 2008, 2010 East Lancashire Hospital NHS Trust. All rights reserved. Can only be reproduced in whole or in part for non-commercial purposes. Not to be reproduced in whole or in part without the acknowledgment of the author and the copyright holder.
