Joint pain and rheumatoid flatfoot
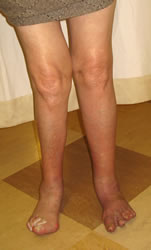
Flatfoot deformity occurs in 25% of patients who have had RA for over 5y
Keenan found a strong association between valgus knee and valgus hindfoot in rheumatoid patients, although she could not establish causality
Patients may have joint pain in the absence of deformity, and this may be difficult to distinguish from ankle joint pain. However, many patients develop a painful flatfoot deformity. Spiegel and Spiegel (1982) reported that 8% of patients who had had RA for less than 5 years had hindfoot deformity, whereas after 5 years the rate was 25%. Bouysset (2002) reported a significant increase in flatfoot deformity after 3-4 years of desease but unfortunately the paper does not present the actual rate of deformity. However, Bouysset (1992) had previously noted that erosions of the talonavicular and naviculocuneiform joints appeared much later, after 10-13y of disease, and that metatarsal erosions were a better marker of impending flatfoot. Hattori (2008), using plain standing radiographs only, described three groups of rheumatoid hindfeet: 64% had neutral feet and no marked joint destruction; 8% had a combination of subtalar and talonavicular joint damage; 27% had predominantly subtalar joint disease.
Keenan (1991) demonstrated reduced movement, velocity and stride length in RA patients compared with normal controls, more marked in patients with valgus deformity. Valgus foot and knee deformities were correlated, but it was impossible to demonstrate causality. Keenan found overactivity in tibialis posterior and no clinical evidence of rupture. However, Bouysset (1995) found tibialis posterior abnormalities on MRI in 1/3 of patients with RA, including 3 ruptures, and Jernberg (1999) found tibialis posterior tendonopathy in 5% of neutral RA feel and 74% of RA flatfeet.
Hindfoot deformity increases medial forefoot pressures and adversely affects the outcome of forefoot surgery (Stockley 1990).
Orthoses
Orthotic devices could be used for correction or support. In particular, they might be used to treat the flatfoot deformity and limit progression, given that orthotic treatment is successful in up to 80% of patients with degenerative adult acquired flatfoot.
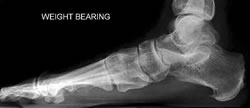
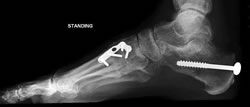
Although Toolan suggested extending the experience of degenerate flatfoot correction to the rheumatoid foot, no series have yet emerged. Calcaneal osteotomy and first ray stabilisation would be a plausible method.
Bouysset (1992) recommended the prescription of orthotics when metatarsal erosions appear, as he found this paralleled the onset of flatfoot; however, no data on effectiveness was provided. Woodburn (2003) demonstrated improvement in hindfoot kinematics over the first year of use of custom orthoses. Hennessy’s (2012) meta-analysis found weak evidence for improvement in pain with custom orthoses, limited by the low quality of many studies. This paper did not differentiate between orthotics for hindfoot and forefoot problems, although of course many rheumatoid patients have both.
Surgery
Toolan and Hansen (1998) recommended functional reconstruction of the rheumatoid flatfoot, drawing on evidence from the management of the degenerative adult acquired flatfoot. However, they did not present any data, and no subsequent series of joint-sparing surgery in the hind/midfoot have appeared.
Triple fusion
The tradition has been to fuse the subtalar, talonavicular and calcaneocuboid joints together on the grounds that this may be required for stability and unfused joints in inflammatory arthritis are likely to require subsequent fusion. Figgie et al (1993) reported 40 triple arthrodeses in RA, with 5% non-union. Eight patients united in >10deg valgus, of whom 5 had ankle pain and 3 had undergone ankle fusion. Knupp (2008) reported 24 triple fusions in 20 patients with RA. All had flatfoot deformity. There were no non-unions or malunions, but 8 patients had superficial wound infections. Arthritis had progressed in 15 midfeet and 10 ankles, but this did not affect outcome. The mean VAS pain score was 47/100, AOFAS midfoot score 70/100 and short musculoskeletal function instrument 45 for dysfunction and 38 for bother. SF-36 scores were just below normal values. Flatfoot deformity may require quite extensive joint resections and medial column shortening (Henderson et al 2002). Stabilisation with compression screws or staples produce similar reported rates of union and clinical benefit. Hindfoot fusion may be combined with ankle replacement to deal with multi-level disease (Kim 2010).
Medial approach to the hindfoot
After correcting a severe flatfoot deformity by triple fusion, it may be difficult to close the lateral hindfoot wound. An alternative is to use a single medial incision (Jeng 2005, Knupp 2009, Weinraub 2010). In these patients the posterior tibial tendon, which normally obstructs the approach, is attenuated or absent. All three joints can be fused through this approach, although Sammarco (2006) showed in a mixed population that subtalar/talonavicular fusion produces satisfactory results and avoids the most challenging part of the procedure.
Isolated joint fusions
Popelka (2010) reported 26 isolated talonavicular fusions in patients with RA, talonavicular joint destruction and tibialis posterior insufficiency. At a mean follow-up of 4.5y, mean AOFAS midfoot score improved from 48.2 to 88.6/100. There was one non-union. Eight patients continued to have pain in the foot, two severe. Joint disease progressed in one subtalar and one calcaneocuboid joint. This series implies that isolated fusion can work even in patients with RA, although there are some uncertainties in the resporting of this series that make generalisation difficult.
© 2008, 2010 East Lancashire Hospital NHS Trust. All rights reserved. Can only be reproduced in whole or in part for non-commercial purposes. Not to be reproduced in whole or in part without the acknowledgment of the author and the copyright holder.
