The debate between surgical and non-surgical treatment of Achilles tendon rupture has pointed first one way, then the other. The introduction, over the last decade, of functional treatment both after surgery and without surgery, has led to a reappraisal of best practice.
Non-surgical treatment
Traditional non-surgical treatment involved extended periods of time in cast, often above the knee initially. The introduction of functional post-operative care stimulated interest in more functional non-surgical treatment methods.
A variety of braces and dynamised casting techniques have been described (Saleh 1992, Thermann 1995, McComis 1997, Roberts 2001, Wallace 2004, Costa 2006, Twaddle 2007, Metz 2008). Weight-bearing has usually been allowed within 2-3 weeks; Costa allowed weightbearing immediately after injury. Active movement with restriction of dorsiflexion has been commenced within days after injury (Costa) to 4 weeks (Roberts, Wallace).
The average re-rupture rate in 8 series which included early weightbearing and functional movement without surgery was 5.5%. Two other series, in which immediate weightbearing was allowed in a cast, had an average re-rupture rate of 7.0%.
Hufner (2006) emphasised the importance of ultrasound monitoring during functional non-operative treatment.
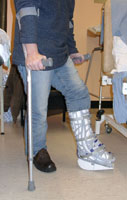
A walker boot allows early weightbearing mobilisation and protected movement. Other splints and functional casting methods have been described
Protected active exercise using the front of the boot to prevent excessive dorsiflexion
Modern functional post-operative and non-surgical treatment of Achilles tendon rupture
Surgery
Open repair
Open repair may be done through a midline, medial or lateral incision. A midline incision gives excellent access but may have more wound problems. By positioning the incision in the sulcus just anterior to the tendon access is still adequate but the wound is less troublesome. The medial approach avoids the sural nerve, while the lateral allows the nerve to be directly visualised and protected.
The tendon is repaired with a suitable tendon grasping suture. The Kessler and Krackow techniques have been described but not compared. Multiple strands of suture increase repair strength but have not yet been shown to improve results.
If possible, a paratenon repair protects the tendon repair from adhering to the wound.
Percutaneous repair
Percutaneous repair minimises the risk of wound complications, but has a risk of sural nerve injury. This has been reported to be as high as 60%, although 5-10% is more representative. Webb and Bannister (1999) described a technique with a posterior rather than lateral portal to avoid sural nerve injury; they had no sural nerve injuries in 27 patients, although one had a regional pain syndrome. Interestingly, Lim (2001) found sural nerve deficits in 7 of 66 patients before surgery, so it is worth making this part of routine initial examination.
Jigs are now appearing on the market to aid suture placement and reduce the risk of nerve injury. Aktas (2009) reported a small RCT comparing open repair with the Krakow technique and minimally invasive repair with the Achillon device. Twenty patients were included in each group. Mean AOFAS hindfoot score was similar in each group (98.7/100 in the Krakow group, 96.7 in the Achillon group) but 7/20 in the Krakow group and 1/20 in the Achillon group had significant soft tissue complications. The randomisation process was poorly described and the assessor was not blinded. Calder (2006) also reported no soft tissue complications and similarly high functional scores with the Achillon technique.
Post-operative management
Carter described free active motion of the ankle after tendon repair in 1992, with excellent functional results and no re-ruptures. Cetti (1994) reported the results of an RCT comparing functional and cast treatment following repair. The functional results were better in the the functional group, with no increase in re-rupture. Khan's meta-analysis of the treatment of Achilles tendon rupture found lower rates of re-rupture and other complications after functional rather than cast treatment. Suchak (2006) performed a meta-analysis of post-operative regimes and found more good results in those treated functionally, without any increase in re-rupture rate. Functional aftertreatment should now probably be considered best practice and casting for the traditional 6-8 weeks can no longer be justified for the average patient provided the necessary facilities and expertise are available.
Yotsumoto (2010) described a brace-free rehabilitation protocol in 20 patients who had surgical repair with a fibrewire suture reinforced with cross-sutures. Non-weightbearing exercise was strted immediately post-operatively. Partial weightbearing was allowed at 1 week and full weightbearing at 4 weeks. There were no re-ruptures, infections or nerve injuries. The mean Achilles tendon rupture score was 74.8/100 at 4 weeks and 98.3 at 24 weeks. On average patients took 15.4 weeks to return to sports. This technique avoids the cost of a brace. The series was small and some safety issues remain. An RCT would clarify rates of re-rupture and speed of recover relative to brace protection and whether more conventional suture methods could allow brace-free rehabilitation.
Comparisons
A number of randomised controlled trials were meta-analysed by Bhandari (2002) and Khan (2005); slightly different criteria meant that slightly different papers were included. Khan found that the rate of re-rupture was 3.5% after surgical repair and 12.6% after non-surgical repair, while the rate of wound infection was 4.1% in surgically treated patients and absent in those non-surgically treated. Bhandari reported similar figures.
Kocher (2002) reported a decision analysis using values similar to those above, with utilities drawn from a population of 30-50 year old men attending a sports medicine clinic for other problems. They found that surgery gave the highest utility value, although the difference was not large. The most significant factors were the probability of complications after surgery and the utility assigned to a re-rupture by the patients - the worse an outcome the patient considered a re-rupture to be, the more likely the analysis was to favour surgery. This is consistent with our experience - the commonest question our patients ask us is "How bad is a re-rupture - can it be sorted?"
However, in almost all the trials analysed by Bhandari, Kocher and Khan, the non-surgically treated patients were splinted in plaster with varying periods of non-weightbearing, and most trials used similar splintage as surgical aftercare. Given the evidence from animal studies and the treatment of tendon injuries in the hand that early movement improves function, it would seem worthwhile to look at the results of functional treatment undiluted by more historical data.
There are 3 RCTs comparing surgical repair (two open, one percutaneous) followed by functional aftercare with functional non-surgical treatment (Thermann 1995, Webb 2000, Twaddle 2007). All of these have some methodological issues and none are large, so should probably be considered level 2 rather than level 1 evidence. Nevertheless none showed any difference in functional outcome between surgical and non-surgical treatment. The re-rupture rate was 3.8% in surgically treated patients and 5.7% in non-surgically treated patients; the wound infection rate was 3.8%. It is interesting that the non-surgical re-rupture rate was less than half that of the pooled trial data.
Examining the re-rupture rates in case series of non-surgical functional treatment produces a rate of 33/548 (6.0%). In series of functional post-operative care it was 19/641 (3.0%). Perhaps the advantage of surgery in avoiding re-ruptures is less than was thought - these figures suggest 33 patients need to have surgery to avoid one re-rupture.
Interestingly, Moller (2001)reported a RCT in which the re-rupture rate was 1.7% after surgery and 20.8% after non-surgical treatment - an impressive difference, but the surgically treated patients had post-op care in a functional brace with weightbearing and active exercise after 2 weeks, whereas the non-surgically treated patients wore a cast for 8 weeks and were nonweightbearing for 4 weeks. Perhaps the difference in re-ruptures was more to do with after-care than surgery?
Larger RCTs of modern care with better methodology are required. In the meantime, we currently use surgical and non-surgical treatment regimes based on those of Webb et al, using a walker boot in which the patient can do protected exercises with the front flap of the boot to block excessive dorsiflexion. We advise patients that non-surgical treatment probably has a higher risk of re-rupture and may produce a slightly weaker calf, but avoids the complications of surgery and that overall the functional results are similar for most patients. We find that about 1/3 opt for surgery and 2/3 for non-surgical treatment, with the main determinant being level of sporting activity.
Delayed reconstruction
A few patients present for treatment weeks or even months after rupture, or sustain a re-rupture. Occasionally, they have little functional deficit and surgery seems to have little to offer. Either surgical or non-surgical treatment may be used. All trials of non-surgical treatment exclude patients more than 1-2 weeks from injury so their results cannot be applied to late presentations or re-ruptures, so surgery is often advised.
Small gaps can generally be closed either by primary suture or a turn-down flap. Gaps from 3-6cm can usually be closed by a turn-down flap or a V-Y advancement of the tendon (larger gaps may be closed with these techniques depending on the quality and amount of gastrocnemius aponeurosis available - our record is 15cm - but this cannot necessarily be relied on and we always ask patients for consent to FHL transfer).
Larger gaps usually require a tendon transfer or the use of artificial implants (Jennings and Sefton 2002). The main donor options are the plantaris, peroneus longus or flexor hallucis longus. FHL has the advantage of being in phase with the Achilles tendon, is stronger than peroneus brevis and readily harvested. The donor site deficit is not functionally significant (Coull 2003). Plantaris is readily available but small; weave techniques have been described but enough tendon is not always available.
The results of late repair are not much, if at all, inferior to those of primary repair (Boyden et al 1995), although Boyden found that no repair restores the full strength of the Achilles tendon. This does allow us to ressure our patients that, in the event of a re-rupture they can still obtain acceptable results.
