This zone runs from the proximal end of the joint between the 4th and 5th metatarsals (the 4:5 joint) to just distal to this joint. Fractures here may be acute or stress fractures.
"True Jones fractures" - a real entity?
In 1993, Lawrence and Botte wrote a review paper which suggested (without any specific analysis of the evidence) that fractures in this region should be divided into "true Jones" and stress fractures. Subsequent work suggests "true Jones" fractures are caused by adduction forces on the forefoot. It is difficult to know whether these are really distinct groups, partly because of the different definitions (and lack of definitions) used. However, Chuckpaiwong (2007) analysed a series of fractures in the metaphyseal/diaphyseal junction region and found no difference in the epidemiology, outcome or risk of non-union between fractures within the 4th/5th intermetatarsal joint and those extending beyond it (this study is discussed in greater detail on the classification page).
There is little information on the outcome or treatment of the "Jones fracture", partly because they are not always distinguished from diaphyseal stress fractures. Konkel reported 10, but did not separate their treatment from other groups. There were 2 delayed unions but no non-unions. Portland et al included these fractures in their study of primary screw fixation. All united in a mean time of 6.2 weeks.
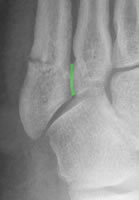
The 4:5 intermetatarsal joint
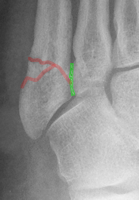
This fracture runs into the 4:5 joint: true Jones fracture according to Lawrence and Botte
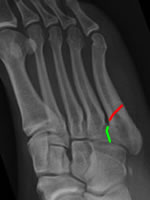
This fracture meets the medial cortex distal to the 4;5 joint: stress fracture
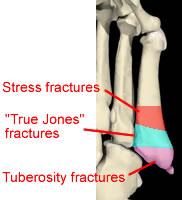
Proximal fracture types according to Lawrence and Botte, based on the relationship of the medial end of the fracture line to the 4:5 joint
Stress fractures
Stress fractures occur mainly in athletes between 15 and 25. Basketball players may be particularly prone to this injury.
Torg subclassified stress fractures into:
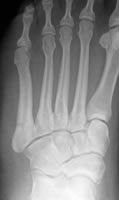
acute fractures with no prodromal symptoms, sharp fracture margins and minimal cortical hypertrophy
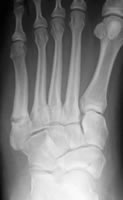
delayed unions with previous injury, widened fracture line, cortical hypertrophy and medullary sclerosis
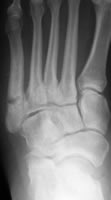
non-unions with wide radiolucency at the fracture line and obliteration of the medullary canal
Non-surgical management
Torg (1984), Zogby (1987), Clapper (1995) and Acker (1986) showed that most “acute” stress fractures will heal in a cast, although healing times may be very prolonged – the median time to union was 21 weeks in Clapper’s study and 11 months in Torg’s initial series.
Torg found that patients kept non-weightbearing initially (mean time of 6 weeks) were more likely to unite and did so quicker than those who bore weight immediately. Even delayed unions may heal in cast – 8/12 in Torg’s series, although the mean time to union was 14 months.
Furia (2010) described a series of patients with non-unions of the proximal 5th metatarsal (no more precise definition). 23 had been treated with shockwave therapy under GA, using an Ossatron or Orthowave-280 device, 2-4000 pulses with an energy flux density of 0.35mJ/mm2. 20 patients were treated with screw fixation. Allocation to treatment was according to which physician was treating. After shockwave treatment patients wore a weightbearing cast for 4-6 weeks, while after surgery they wore a NWB splint for 2 weeks and a stiff shoe for 2 weeks. The main oucome was fracture healing, determined by independent radiograph assessment and clinical criteria. After 6 months, two fractures in each group were not united. One patient in the shockwave group had petechie in the foot; in the fixation group, 7 patients had screw impingement on the cuboid, one an infection and one a re-fracture. There was no untreated group to control for the possibility that fractures might have healed without the study interventions, and possible issues wth independence of treatment. An RCT is really needed to evaluate the place of shockwave treatment rigorously.
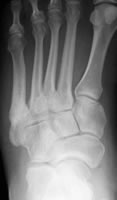
This stress fracture healed after 2.5 years (patient declined surgery)
Surgery
Mologne et al (2005) reported the first RCT comparing medullary screw fixation with casting. Although the numbers were small, there was a large and significant difference in outcome between the groups. The surgical group united in a mean of 7.5 weeks and returned to sport at 8 weeks, with one non-union. The non-surgical group united in a mean of 14.5 weeks and returned to sport at 15 weeks, with 5 non-unions.
Based on these results, surgery should be offered at least to young, physically active patients with stress fractures. Casting remains an acceptable option for patients who prefer it.
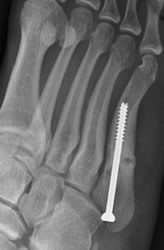
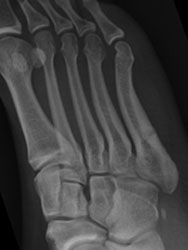
Stress fracture in semi-professional footballer; healed in 7 weeks after cannulated screw fixation
Intramedullary screw fixation is the method most commonly reported. Comparisons between 4.5mm, 5mm and 6.5mm screws have not shown reproducible clinical or biomechanical differences.
Kelly et al (2001) found pullout strength for 6.5mm screws better than 5mm. However, Shah et al (2001) found no difference and commented that larger screws could increase the risk of intra-operative or post-operative fracture. Wright et al (2000) suggested using large diameter screws in athletic patients with high body mass
Mologne et al used 4.5mm screws in their RCT.
Tension band wire and plate fixation have also been reported.
