Fractures of the medial malleolus usually occur in association with fractures of the lateral and, less commonly, posterior malleolus. Issues around the management of such injuries are mainly dealt with in the pages on displaced ankle fractures.
The presence of a medial malleolar fracture is sometimes taken as an indication to operate on a displaced ankle fracture because of a perceived risk of symptomatic medial malleolar non-union. In fact this risk seems lower than is often thought. In the four randomised controlled trials of the management of displaced ankle fractures there were no symptomatic medial malleolar non-unions in about 300 patients treated with closed reduction and casting.
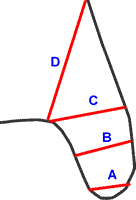
Herscovici classification of medial malleolar fractures.
- A - tip avulsions (anterior colliculus)
- B - intermediate
- C - level of plafond
- D - above plafond (adduction fractures)
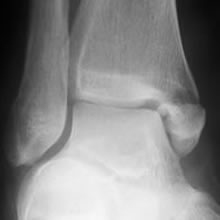
Undisplaced medial malleolar fracture (Herscovici type C). Think - could there be a missed proximal fibular or syndesmosis injury?
Isolated fractures of the medial malleolus do occur. Herscovici (2007) reported 67 isolated medial malleolar fractures, all treated in cast. All but two united, even in the presence of an average of 3mm displacement. Before deciding a medial fracture is isolated, look for an occult injury, especially to the proximal tibio-fibular joint, the proximal fibula or the syndesmotic ligaments, which would render the ankle complex unstable.
Herscovici produced a classification of medial malleolar fractures by level, drawing on previous classifications:
- Type A are small avulsions which may carry a significant part of the superficial deltoid ligament. They represent avulsions of the anterior colliculus. The deep deltoid, however, is attached more posteriorly, mainly to the posterior colliculus. Therefore, if there is a small, type A fracture of the medial malleolus associated with displacement of the talus in the mortise, the deep deltoid must also be torn (as otherwise it would prevent the talus moving away from the non-fractured part of the malleolus. In this situation, fixing the malleolar fragment will not restore ankle stability.
- Type B and C fractures are mainly associated with external rotation and abduction fractures in the Lauge-Hansen classification system (types B and C in the AO/Weber classification). They are basically avulsion injuries. Osteosynthesis of these fractures will be stressed in tension. The usual fixation methods are compression screws (using two if possible to prevent rotation), or tension band wiring. Two studies suggest that tension band wiring is better at resisting pronatory forces on the fixation construct, although no clinical study has shown a difference in outcome between the two techniques. Both seem acceptable methods to use.
- Type D fractures are mainly associated with supination-adduction type injuries (type A in the AO/Weber classification). They are quite uncommon injuries: 1/6 of Herscovici's series and only 5% of McConnell's. They are impaction injuries which may produce some longitudinal instability. 8/19 vertical fractures in McConnell's series had some degree of impaction of the plafond adjacent to the main fracture line. This is a serious injury which requires reduction of the plafond impaction and stable fixation. Bone grafting of the impacted area is usually recommended. Toolan (1984) found that the most stable form of fixation of adduction fractures was cancellous lag screws perpendicular to the fracture site. Anti-glide plates provided much less stability. Dumigan (2006) recommended the use of a neutralisation plate. Both of these studies were carried out on cadavers; there are no comparative clinical studies.
Some medial malleolar fractures extend posteriorly into the posterior margin of the plafond. In Haraguchi's (2006) study of posterior marginal fractures, 20% involved the medial malleolus. Weber (2004) drew attention to these fractures, and to the need for more extensive exposure to allow reduction and stabilisation, often with a small posterior plate. Klammer (2013) extended this description, linking it with the Haraguchi type 2 fracture and indicating which fractures could be treated through a posterolateral incision and which required a medial approach also.
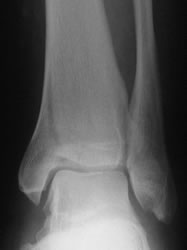
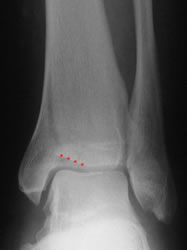
Adduction fracture of the medial malleolus. Note the adjacent plafond impaction (marked)
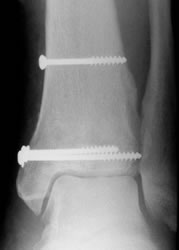
After reduction and bone grafting of the impacted joint surface and stabilisation with cancellous lag screws
