Fractures of the posterior malleolus almost always occur in association with a fracture of the lateral malleolus and a medial injury. “Isolated” posterior malleolar fracture should lead to suspicion of a proximal fibular (Maisoneuve) fracture and/or a major soft tissue disruption.
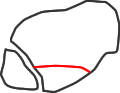
type 1
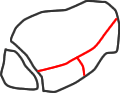
type 2
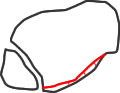
type 3
Haraguchi CT classification of posterior malleolar fracture morphology (see text)
Haraguchi et al (2006), using CT, found that 2/3 of posterior malleolar fractures were wedge-shaped and related to the posterior tibiofibular ligament, but 20% were transverse, extending in to the medial malleolus, and 15% were small posterior shell fragments. Weber (2004) described a postero- medial fracture variant and Klammer (2013) extended this description, linking it with the Haraguchi type 2 fracture and indicating which fractures could be treated through a posterolateral incision and which required a medial approach also.
A number of biomechanical studies suggest that tibiotalar instability occurs with a posterior fracture that separates 30-40% of the joint surface, in the posterolateral position, from the rest of the plafond. It is difficult to measure the proportion of separated joint surface from plain Xrays, as the fracture line is usually oblique. Ebraheim et al (1999) recommended the use of external rotation lateral views, although Haraguchi et al (2006) found that the angle between the fracture and coronal plane varied unpredictably from -9 to 40 deg. Some studies suggest that adequate reduction of the fibula or an intact DTTL can prevent instability.
Clinical studies, however, have not shown a clear proportion of posterior separation that predicts a poor result. Both Harper (1988) and Jaskulka (1989) found that outcome was determined by the overall severity of the fracture and the adequacy of reduction, and Tejwani (2010) found that the presence of a posterior malleolar fracture of any size predicted poorer outcome for an ankle fracture, perhaps indicating a higher-energy injury. Mingo-Robinet (2011) found that results were poorer in patients with a posterior malleolar fragment greater than 25% on lateral Xrays, but the quality of reduction did not have a significant effect and they did not analyse the effect of different sizes of posterior fragment. At the moment we still recommend fixation of a large posterior malleolar fragment (over 25%), and if this requires open reduction we would now use the posterolateral approach in view of the experience in association with syndesmotic injuries.
Recent studies have explored the importance of the posterior malleolus in syndesmotic injuries. Gardner (2006) demonstrated in a cadaver model that posterior malleolar fixation restored 70% of syndesmosis stablity compared with 40% after syndesmotic screw insertion. Miller (2010) then demonstrated, in a small series, that open reduction and stabilisation of the syndesmosis produced equivalent clinical results to syndesmosis screw fixation. They recommended (Miller 2009a) direct visual confirmation of syndesmotic reduction and described the use of the posterolateral approach to achieve this (Miller 2009b). By using this method they reduced the rate of syndesmotic malreduction from 52% (Gardner 2006, Miller 2009) to 16% (Miller 2009). Amorosa (2010) reported a similar improvement in anatomical reduction from 27% with indirect reduction to 83% with direct open reduction.
Many smaller posterior malleolar fractures can probably be treated with indirect reduction but the posterolateral approach is a useful part of the ankle fracture surgeon’s toolbox.
