About 75% of ankle fractures are undisplaced at presentation. "Undisplaced" means the talus is congruent in the mortise, although there may be small amounts of displacement of malleolar fragments. In the majority of these there is sufficient deep deltoid ligament function to prevent displacement. Overall the likelihood of the fracture behaving in a stable manner is:
- No medial tenderness, bruising or swelling >99%
- Medial tenderness, bruising or swelling 90-98%
If in doubt weightbearing stress radiographs (mortise and lateral) are probably the most useful way of identifying the small number of undisplaced, unstable fractures (Hoshino 2012).
Undisplaced, stable fractures
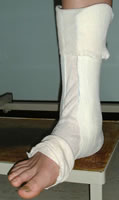
Focused rigidity casting (FRC) ankle brace - cheap and easy to produce, fits in a trainer.
These fractures make up about 50-70% of all ankle fractures (Fox 2005, Koval 2007). They have a functioning deep deltoid ligament (Michelson 1996).
An RCT by Stuart (1989) compared cast with Aircast brace for the treatment of stable ankle fractures, and a further RCT by Port (1996) compared cast with bandage. In both these studies, patients treated without cast had less pain and stiffness initially, although by 6 months the casted fractures had caught up. A further trial by Brink (1996) showed no advantage of a walker boot over an Aircast brace. All fractures in these three trials healed in the normal time whether a cast was used or not, and none of them had any weightbearing restrictions. This confirms the biomechanical evidence that stable fractures do not displace under normal loading (Michelson 1995, 1996).
Thus stable fractures do not need a cast to achieve healing in a good position. If anything, patients treated in cast recover function and comfort more quickly. However, it is sometimes said that patients require a cast for pain control. Dalal (2010) reported that, given an informed choice, 82% of patients chose a brace, 17% RICE and 1% a cast.
There is no need to restrict weightbearing. Follow-up radiographs are not necessary (Michelson 1995) and given adequate initial assessment, fracture clinic attendance is not required (Martin 2004).
"Borderline" fractures
Stable fractures are usually readily apparent. However, some patients have reasons to suspect possible instability even when the initial radiograph is undisplaced, including:
- medial tenderness, bruising or swelling
- fibular fracture above the syndesmosis
- higher energy injury
For some years the standard test was an external rotation stress radiograph (McConnell 2004, Egol 2004, Schock 2006). However, Koval (2007), Tornetta (2012) and Hoshino (2012) showed that even in the presence of a positive external rotation stress test conservative treatment in a brace or cast usually produced union in an undisplaced postion. Koval found late displacement in 1/19 patients, Hoshino in 3/38 and Tornetta in 0/54. Akhtar (2009), whose series began before stress radiography was popularised, described displacement in 3/153 patients with clinical risk factors. In Akhtar's series, all displacements occurred in the first week, and all who had normal weightbearing radiographs at 1 week united without displacement. These data suggest the risk of displacement is low. However, Sanders (2012) randomised patients with a positive stress radiograph to surgical fixation or cast. There was no difference in functional outcome, but 20% of conservatively treated patients displaced, two of whom were operated on.
The cut-off between stable and non-stable fractures has not yet been fully defined, but clinical features and weightbearing radiographs seem to define the large majority. Further studies are required. However, in the meantime the important management goal should be to avoid casting and weightbearing restrictions in the large group where stability is not controversial.
