Syndesmosis injuries are, generally, the most severe ankle fractures, with high risks of dislocation and joint surface injury. Egol (2009) found that the functional outcome of patients who required syn- desmotic stabilisation was worse than those who needed only malleolar stabilisation.
Syndesmotic injury is usually associated with supra-syndesmotic fracture, but the level of the fracture does not predict the level of the tear of the interosseous membrane very accurately (Nielson 2004, Hermans 2011), so some fractures will be more unstable than the radiograph suggests. Indeed, Stark (2007) found that intra-operative stress testing identified syndesmotic injuries in 38% of trans-syn- desmotic (AO type B) fractures, although their diagnostic criteria for a stable syndesmosis were quite stringent.
Black (2013) found that CT changed management in 40% of syndesmosis injuries.
The syndesmosis presents a complex appearance on plain Xray. Three measurements have been studied, and were entitled “syndesmoses A-C” by Pettrone et al (1983):
- Syndesmosis A (also known as the tibio-fibular clear space) is measured on the AP radiograph between the lateral border of the posterior malleolus and the medial border of the fibula. There was a small but significant difference in the outcome scores between patients in Pettrone’s series with a post-reduction value of 5mm or more and those less than 5mm, and so this was considered abnormal.
- Syndesmosis B (also known as the tibio-fibular overlap) is measured on the AP radiograph between the medial border of the fibula and the lateral border of the anterior tibial prominence. There was a small but significant difference in the outcome scores between patients with a post-reduction value of 10mm or more and those less than 10mm, and so this was considered abnormal.
- Syndesmosis C was the same measurement as syndesmosis B, but on the mortise radiograph. A value of 1mm or less was considered abnormal
- The medial clear space also gives indirect information about the integrity of the syndesmosis, and Nielson (2005) referred to this as “syndesmosis D”. Pettrone considered a medial clear space of 3mm or greater on the AP view to be abnormal. As noted elsewhere, most studies have examined the mortise view, and current evidence suggests 4-5mm as the upper limit of normal.
Brage (1997) found that measurement of the tibiofibular clear space and mortise overlap had relatively poor reproducibility on a standardised set of Xrays, while the AP overlap was highly reproducible. Pneumaticos (2002) found that the tibiofibular clear space was constant irrespective of the rotation of the ankle, while the overlaps and medial clear space were highly rotation-dependent. However, Beumer (2004) found that measurements on cadavers were so position-sensitive that comparison of repeated measures was almost meaningless.
Which fractures need syndesmosis stabilisation?
Biomechanical and clinical studies, particularly those of Boden (1989), clarified these injuries and suggeste selective syndesmotic stabilisation. As with other ankle fractures, an intact deep deltoid ligament would protect against tibio-talar displacement even with severe syndesmotic tears – tears up to 15cm above the ankle have been studied in cadaver experiments. However, if the medial malleolus was fractured or the DTTL torn, a low syndesmotic tear (existing data suggest <4.5cm from the ankle joint line) could still be stable if the fibula is anatomically reduced and fixed. Above this, a syndesmotic positioning screw is likely to be needed. van den Bekerom (2010) confirmed that Boden's criteria had a specificity of 0.96 but a sensitivity of only 0.39: they are good at ruling in the need for a syndesmosis screw but less good at ruling it out.
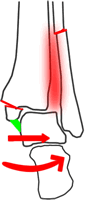
If there is a medial malleolar fracture with the deep deltoid attached...
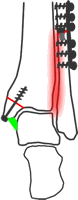
...stable fixation of this should stabilise the fracture, no matter how high the fibular fracture is. A plate would be applied to the fibula if feasible.
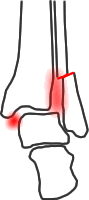
If there is a fibular fracture within 4.5cm of the plafond...
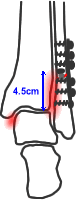
...and the fibula can be fixed in stable configuration, the fracture would normally be stable
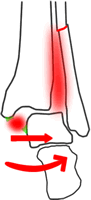
If the fibular fracture is >4.5cm above the plafond...
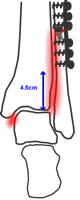
...even stable fixation of the fibula will probably not stabilise the ankle
In each case the construct should be stress-tested (see below)
There are a number of issues in translating these biomechanical studies into real life:
- A clinical study confirmed that if the medial malleolus and the fibula are fixed in a stable manner, the syndesmosis will normally be reduced and stable, and a syndesmotic stabilisation screw will rarely be required.
- However, fibular stabilisation may sometimes be relative in these severe injuries, which often have significant comminution.
- The level of the fracture does not predict the level of the tear of the interosseous membrane very accurately (Nielson 2004), so some fractures will be more unstable than the radiograph suggests. Indeed, there have been a number of papers which suggest that anything up to 30% of even trans-syndesmotic (AO type B) fractures may have significant syndesmotic injuries with residual instability even after ORIF.
- One some times sees small medial malleolar fractures, which usually represent the anterior colliculus of the malleolus only. The deep deltoid is not attached to this, but more posteriorly. Therefore, if the anterior colliculus is fractures and the mortise is incongruent, the deep deltoid ligament must also be torn. Fixation of the medial malleolar fragment in this situation will not stabilise the medial side.
Therefore, it is probably best to stress test all ankle fractures after bony stabilisation. he syndesmosis should be stressed laterally, anteropos- teriorly and in external rotation – Candal-Couto (2004) suggested the main direction of instability is anteroposterior rather than laterally, and Xenos (1995) found that AP radiography correlated less well with measured rotation in cadaver legs than lateral radiography. Radiographic screening is important, although direct palpation of the syndesmosis may also be useful
Both Gardner (2006) and Vasarhelyi (2006) found that over 50% of ankle fractures with syndesmotic injuries showed some degree of malreduction on CT after apparently satisfactory ORIF. Symeonidis (2013) reported a re-operation rate of 27% for missed syndesmosis injuries, malreduction or loww of reduction in a tertiary centre. Although late reconstruction can give good results, it is better to ensure accurate reduction at primary surgery. Recent studies have explored the importance of the posterior malleolus in syndesmotic injuries. Gardner (2006) demonstrated in a cadaver model that posterior malleolar fixation resored 70% of syndesmosis stablity compared with 40% after syndesmotic screw in- sertion. Miller (2010) then demonstrated, in a small series, that open reduction and stabilisation of the syndesmosis produced equivalent clinical results to syndesmosis screw fixation. They recommended (Miller 2009a) direct visual confirmation of syndesmotic reduction and described the use of the poste- rolateral approach to achieve this (Miller 2009b). By using this method they reduced the rate of syndesmotic malreduction from 52% (Gardner 2006, Miller 2009) to 16% (Miller 2009).
Syndesmosis stabilisation techniques
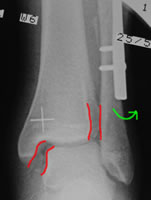
High fibular fracture with deltoid tear. Despite fixation of the fibula with a DCP, stress testing shows residual instability
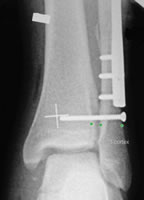
A 3-cortex 3.5mm positioning screw is inserted through three cortices 2cm above the plafond
Biomechanical studies suggest a single 3.5mm cortex screw, through 3 cortices, about 2cm above the ankle joint line, is adequate for stability. Additional, or larger, screws, do not normally resuce the risk of late displacement (Hoiness 2004, Moore 2006, Markoff 2013). It should be a neutral, not a lag screw. Occasionally, however, a second screw is required in a highly-unstable fracture or a very large patient.
The use of a fibre-wire is appealing, as it would potentially allow some natural movement of the syndesmosis. There has been some controversy as to whether the construct is strong enough, but recent cadaver series (Klitzman 2010), suggest syndesmotic movement is close to normal. Case series (Cottom 2009, de Groot 2011) have reported generally positive results, although with significant levels of local complications. Naqvi (2012) compared patients stabilised with tightropes to those with syndesmosis screws, with CT examination of reduction. 23% of screw fixations had malreduction compared with none in patients with tightropes. There were no significant differences in clinical outcomes; the rate of soft tissue complications was not reported. One or more RCTs would be preferable to compare screw and fibrewire fixation.
Should syndesmosis screws be removed?
It is traditionally advised to keep patients with syndesmosis screws non-weightbearing until the screw is removed at 6-12 weeks, lest the screw should loosen or break, usually the former. Hamid (2009) found no difference in AOFAS ankle scores between patients who had retained syndesmosis screws, broken screws and retained screws. However, those with retained screws had slightly higher pain scores. Manjoo (2010) found better Olerud-Molander scores in patients who had screw removal or breakage, than in those with intact screws. The tibiofibular clear space was narrower with intact screws. Hsu (2011) and Tucker (2013) also noted no difference in outcome between patients with broken screws and those with intact screws. Hsu also found that 15% of diastases recurred in patients whose syndesmosis screws were removed before 3 months, although this did not affect clinical outcome with the numbers of patients in their study.
Miller (2010) noted improvements in range of movement and ankle scores after implant removal in 25 patients who had syndesmotic screw and fibular plate removal. It appears that it is intact, rather than broken, screws that can cause difficulties. Manjoo recommended offering screw removal six months after ORIF to patients whose screws are intact at that stage, which seems consistent with current evidence. The evidence on syndesmotic screw removal is summarized in a systematic review by Schepers (2011).
