Clinical features
Most patients have a history of a high-energy axial injury and may have other associated injuries of the calcaneum, knee, hip or spine. Some series report polytrauma in 10-20% and 10-30% open fractures, but these were from level-1 trauma centres. Compartment syndrome of the foot has occasionally been reported after pilon fractures.
Imaging
Full ATLS primary and secondary survey is required for major injuries. Examine for neurovascular injuries, compartment syndrome and associated skeletal injuries. Assess the patient’s overall medical fitness, especially a history of vascular disease, diabetes or inflammatory arthritis and any major medical illness.
Plain AP and lateral radiographs should be obtained, along with imaging of any other associated injuries. Plain films show how proximal the fracture extends and shows overall alignment. they should be carefully studied for evidence of lateral disruption and functional diastasis (Topliss 2005). Other initial investigations are obtained as clinically indicated.
CT is very useful in assessing pilon fractures. It allows one to identify the main fracture fragments and the main fracture line for surgical planning. It also gives the best impression of comminution and joint surface injury. Tournetta (1996) found that CT influenced management in 60% of patients. Except in the emergency situation, we would not operate on a pilon fracture without a CT. Other imaging modalities probably add little to plain films and a CT, although this has not been formally evaluated.
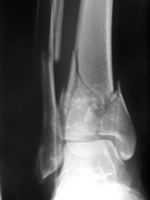
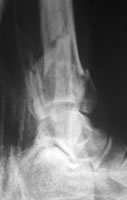
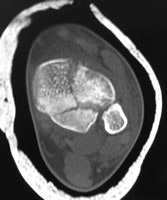
Plain films and CT of pilon fracture: Ruedi-Allgower II, AO C2, Topliss sagittal-Y
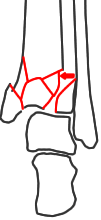
Functional diastasis
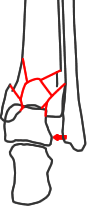
Lateral disruption
