Two main classifications are used, which use different criteria for grouping. A new CT-based classification from Bristol builds on the work of Tournetta and offers important new insights.
Ruedi/Allgower classification
Ruedi and Allgower described three groups based on the size and displacement of articular fragments:
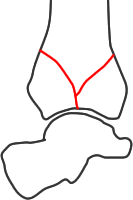
I - no comminution or displacement of joint fragments
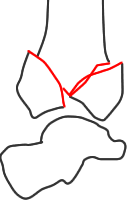
II - some displacement but no comminution or impaction
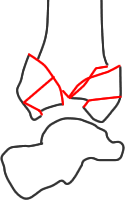
III - comminution and/or impaction of the joint surface
AO classification
The AO long bone group universal classification of fractures groups distal tibia fractures as 43. The first sub-grouping is on the degree of cntinuity between diaphysis and metaphysis:
- 43A: extra-articular – most would not recognise these as pilon fractures, although in some series non-articular fractures are included and it can be difficult to tell how many were articular
- 43B: partial articular fractures with some connection between part of the joint surface and the diaphysis - again, some series appear to include these but most do not clearly differentiate between them and those with complete separation between diaphysis and metaphysis. Posterior partial fracture overlap with malleolar fractures with posterior malleolar components (Klammer 2013), and anterior partial fractures were included by Lauge-Hansen (1950) iin his classification of malleolar fractures
- 43C: complete articular fractures with no connection between the joint surface and diaphysis – most pilon fractures fall into this group
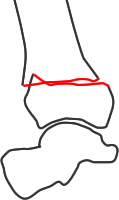
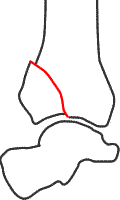
AO group A - extra-articular fracture
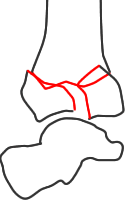
AO group B - partial articular fracture
AO group C - complete articular fracture
There are sub-classifications of each of these groups - the most important being the group C fractures:
- 43C1: no comminution of epiphysis or metaphysis
- 43C2: comminution of metaphysis but not epiphysis
- 43C3: comminution of epiphysis +/- metaphysis (corresponding roughly to Ruedi-Allgower group III, many pilon fractures are in this category)
Both Martin (1997) and Swiontowski (1997) found moderate reproducibility at the A-B-C level but it was poorer at the subgroup level.
Luk (2013) compared pilon fracture types in patients with and without an intact fibula. When the fibula was intact, 58% of fractures were partial articular type B. When the fibula was fractured, nearly 70% were type C complete articular fractures and over half were type C3, the most comminuted.
Topliss classification
Topliss et al (2005) re-examined the anatomy of pilon fractures based on plain radiography and CT. The paper should be read in detail - important points include:
- six typical fragments, recognition of which helps plan reconstruction - not all present in any one patient:
- anterior
- posterior
- medial
- anterolateral
- posterolateral
- die-punch
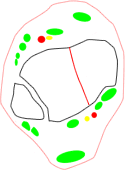
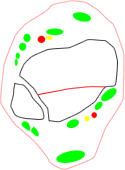
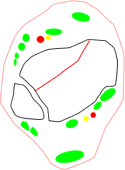
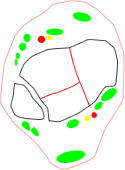
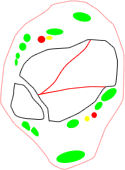
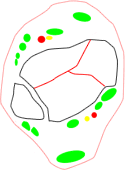
- three main groups of fractures based on the main orientation of the fracture lines:
- coronal group, typically lower-energy fractures in older patients with a more distal metaphyseal-diaphyseal dissociation and valgus alignment (56%)
- sagittal group, typically higher-energy fractures in younger patients with a more proximal metaphyseal-diaphyseal dissociation and varus alignment (33%)
- comminuted fractures of such severity that they could not be assigned to any group (6%)
- a group of fractures ("lateral disruption fractures") with incongruity of the joint between the lateral malleolus and the lateral talar facet, often with an intact fibula. In this group there was always a tibial fragment remaining in the correct relationship to the fibula which could be used to help judge reduction, but failure to recognise and reduce talofibular incongruity led to poor results
- a group of fractures with "functional diastasis" of the tibiofibular articulation because of separation between the main block of distal tibia and fragments still attached to the fibula. Again, failure to recognise and correct this led to poor results.
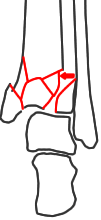
Functional diastasis
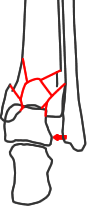
Lateral disruption
energy |
sagittal fracture family |
posterior coronal fracture family |
anterior coronal fracture family |
lower |
 |
 |
 |
higher |
 |
 |
 |
Topliss compared the reproducibility of their grouping with division into AO "B" and "C" groups. The Topliss classification was more reproducible, especially in the hands of Topliss herself, although no statistical analysis is provided. A diagram summarising fracture alignments is provided, which implies very few fracture lines in intermediate positions between the coronal and sagittal families - it would be valuable to reproduce this in a different data set.
Tang (2012) proposed a four-column classification which has some similarities to the Topliss classification but omits central fragments. The authors describe how this influences surgical approach but the data do not clarify this and the classification may need some further development to make a distinct contribution to decision making.
