Initial management includes resuscitation, pain control and splintage. Partial reduction may be indicated to prevent skin breakdown. Open injuries should be documented, cleaned and dressed.
Soft tissue management
There are few better examples than the pilon fracture of the aphorism that a fracture is a soft tissue injury with a broken bone in the middle. The soft tissue envelope of the distal leg has relatively vulnerable blood supply and poor healing capcity, especially in the older patient with medical co-morbidities such as diabetes, vascular disease or lipodermatosclerosis. Fracture blisters and skin necrosis readily develop and wounds may heal poorly. Teeny and Wiss (1993) documented the soft tissue disasters that could result from conventional surgery.
Current surgical techniques aim to minimise disruption of the soft tissue envelope. Methods include:
- temporary stabilisation and delay in definitive surgery until the soft tissues have settled
- joint reconstruction through small incisions directly over the main fracture line
- reattachment of the articular to the metaphyseal fragment with fine-wire fixators or minimal-incision plate osteosynthesis (MIPO)
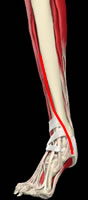
Traditional approach for ORIF - large incision with soft tissue undermining
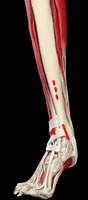
Direct aproach to avoid undermining and incisions for minimal incision plating
Non-surgical management
Non-surgical management in a cast with avoidance of weightbearing in view of the disrupted plafond may be useful in a few undisplaced fractures (Ayeni 1988). Ayeni used plaster for 12 weeks and NWB for 10 weeks; there are no data to show whether such protracted restriction is necessary. Ayeni found that displaced or comminuted fractures did poorly in casts.
Surgical reconstruction
Surgery can be divided into two main groups:
- Open reduction and internal fixation: popularised by Ruedi and Allgower, who emphasised plating the fibula to regain length, reduction of the plafond and bone grafting to support the articular surface followed by medial buttress plating. A long anteromedial incision was used, with undermining to reach the fragments. Unfortunately this has been associated with a high incidence of wound failure. More recently, reduction of the articular surface through a small incision related to the main fracture line without undermining, followed by minimally invasive insertion of a low-profile plate to attach the articular fragment to the shaft has been proposed and reported to have alower incidence of wound problems.
- External fixation to regain length, often with minimally invasive reduction and stabilisation of the articular fragments. Bridging unilateral fixators, hybrid frames and full circular frames have been used.
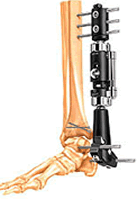
Bridging external fixator
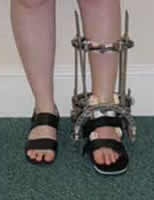
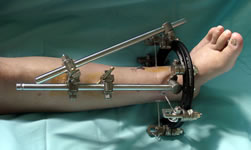
Non-bridging fixators - full ring Ilizarov frame (L), AO hybrid frame (R)
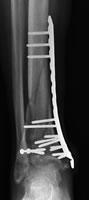
MIPO
Results of surgery
Only one RCT has compared internal and external fixation. Wyrsch et al (1996) reported no difference in clinical outcome, but a higher incidence of severe soft tissue complications in the ORIF group. Allocation to treatment was not truly randomised and there were, in fact, more severe injuries in the external fixation group. The power of the study was low. Fixation was usually performed within the first week when the soft tissues might be expected to be swollen. It is difficult to draw useful conclusions from this study.
Several other retrospective comparative series have been reported (eg Williams 1998, Blauth 2001, Pollak 2003, Koulouvaris 2007, Davidovich 2011) with variable results. In Koulouvaris' series, 20 patients had a monolateral spanning fixator, 22 had a hybrid fixator and 13 a 2-stage ORIF. The spanning fixator patients took longer to achieve union (6.9months vs 5.6 vs 5.1) and were more likely to reduce their activities. However, allocation to treatment was dependent on the treating surgeon and the groups were not entirely comparable. Davidovich (2011) reported 20 patients who had bridging external fixation with minimally invasive reduction and fixation of joint fragments, plus 26 who had conventional ORIF. AOFAS and SMFA scores, range of movement, complications and prevalence of arthritis were similar in both groups. ORIF patients waited longer for surgery and had more secodnary procedures.
Papadokostakis et al (2008) give an excellent systematic review of the literature on external fixation. They concluded that the results of bridging and non-bridging fixators was similar; there was a higher risk of malunion in the bridging series but this could be due to confounding factors such as initial fracture severity.
Series reporting the results of external fixation include Watson (2000) – Ilizarov frame for severe soft tissue injuries only, Angelen (2001), Blauth (2001) – historical comparison group for minimally invasive plating, Tornetta (2003), Okcu and Aktuglu (2004), Williams (2004) and Pollak (2004). The results vary widely, partly because some series selected more severe fractures for external fixation. Most series carried out limited open reduction and screw fixation of the joint surface in addition to external fixation, and a variety of frame configurations were used. Okcu and Aktuglu compared transarticular and non-bridging Ilizarov frames retrospectively; the Ilizarov group got a better range of movement but the Olerud ankle scores were similar. Williams compared external fixation with and without fibular plating; fibular plating prevented malunion but at the cost of many lateral wound complications, and the malunions were asymptomatic – Williams recommended a selective approach to fibular plating. In most series the rate of wound infection with fixators was lower than in ORIF and pin track infection rates were manageable. Malunion rates vary from 4-20% and some series report a number of metaphyseal-diaphyseal non-unions.
Series reporting the results of traditional ORIF include Ruedi and Allgower (1988), Teeny and Wiss (1993), Watson (2000) – for mild soft tissue injuries only - Paterson and Cole (1999) and White (2010). Teeny and Wiss were among the first to draw attention to the high rate of wound problems in high energy injuries fixed by the methods of Ruedi and Allgower – half their grade III injuries had poor clinical results due to a combination of inadequate reduction, malunion (23%), non-union (27%) and infection. Restricting ORIF to those with mild soft tissue injuries (Tscherne grades 0-1), Watson reported 14% wound failure, 5% deep infection, 11% non-union and 4% malunion. Both Paterson and Cole and Blauth advocated temporary external fixation or traction with delayed ORIF at about 14 days (Blauth also used minimally-invasive plating rather than the traditional technique). Paterson and Cole’s series consisted of 22 AO 43C3 fractures only but they had no wound problems or deep infections, one malunion and one non-union. Blauth had a 12% infection rate but no malunion or non-union. Syed and Panchbani described a percutaneous screw technique which is applicable in Ruedi/Allgower I and II fractures and avoids wound problems without significant bone healing problems in a small series.
More recent series (eg Blauth 2001, Syed and Panchbani 2004, Bahari 2007, Leonard 2009, Collinge 2010, Tong 2012) have focused on the use of minimally invasive reconstruction and plate fixation, often using anatomically designed and/or locking plates. Overall, these series report rates of non-union, mal-union and infection of around 5%. There is a need for RCTs comparing modern plating and external fixation techniques. Locking plates have become popular, but there have been concerns that the very stiff constructs they create might delay union. Ozkaya (2009) compared the time to union in 21 patients stabilised with a steel non-locking plate and 22 treated with a titanium locking plate. (All fractures were extra-articular so were not true pilon fractures, but could shed light on the more severe fracture types.) The groups were otherwise comparable. The mean time to union in patients with locked plates was 18 weeks and with non-locked plates 15 weeks. There were one non-union and two delayed unions in the locked group and none in the non-locked group. Overall clinical outcome, however, was comparable.
Boraiah (2010) reported 59 patients with open pilon fractures. These were seriously injured patients - mean injury severity score was 18 and 59% had multiple injuries. 63% had Gustillo/Anderson grade 3A injuries and 29% grade 3B (no grade 3C). All had standard wound debridement and most had temporary delta-frame spanning external fixation. Definitive stabilisation was with minimal incision screw and mini-plate fixation, and 17 had free muscle flaps. There were six non-unions, all with segmental bone loss, which healed with late grafting. One patient had an amputation due to flap failure. There were two deep and three superficial infections. SF-36 physical scores in 38 pateints followed for more than 2 years were slightly lower than norms and mental scores above norms. The mean modified Mazur score, however, was 44.8/100. Gardner (2008) described 1 patients with open AO type C3 fractures with bone loss treated with a staged protocol: stage 1 was debridement and spanning fixation, stage 2 plate fixation and antibiotic bead placement and stage 3 bone grafting of the defect. 9/10 healed; there were 2 deep infections and one amputation.
Bozic reported 15 pilon fractures which were considered unreconstructable and were treated by primary ankle fusion. These represented 5% of the pilon fractures treated by the unit in the study period. Eight fractures were open and 5 had metaphyseal bony defects. A posterior approach with iliac crest graft was used. All fractures united, although one plate broke before union was achieved. There was one deep infection. This offers a potential "bail-out" for very severe injuries. Niikura (2009) used an antegrade tibial nail to carry out primary ankle fusion in two similar patients, both psychotic.Both fusions united and the patients were pain-free at 2 years post-op.
There is debate on whether it is necessary to fix a fractured fibula in association with a pilon fracture. The argument is that it supports the tibia out to length and mayprevent mal-union. On the other hand, there is concern that its rigidity could precipitate non-union or varus deformity of the tibia. Williams (1998) reported 54 pilon fractures treated with monolateral bridging external fiation, of which 22 had the fibula fixed and 32 did not. The patients with fibular fixation were less likely to get tibial angulation (1 case vs 6), but at the cost of additional wound and healing complication related to the fibular surgery. Overall there was no difference in results. On the other hand, Lee (2009) found that patients who had fibular stabilisation in association with tibial plating had a trend to better results than patients in whom the fibula was left alone; however, the differences were not significant.
An alternative method of initial stablisation was described by Ketz (2012). For patients with type C fractures and a posterior malleolar fragment they initially stabilised the posterior malleolus through a posterolateral approach followed by anteror ORIF after an interval. These were compared with a group who had a standard anterior approach. The patients who had an anterior approach were more likely to have articular incongruity and joint space narrowing, and both subsequent fusons occurred in the anterior group.
At the moment bridging, hybrid or circular external fixation, or delayed ORIF, possibly with minimally invasive plating, can all be justified for the management of pilon fractures. Techniques for both internal and external fixation have improved since Wyrsch’s RCT, and further large trials with better methodology, perhaps across several centres to get adequate numbers, would be justified. However, these are quite heterogenous fractures, and it may be difficult to apply the results of even quite a large trial. It may be that several options will continue to have a place, with each surgeon being responsible to monitor their own complications.
Outcomes
A number of series (Marsh 2003, Pollak 2003, Williams 2004) have concentrated on the overall clinical outcomes of pilon fractures, using general outcome measures such as the SF-36 as well as ankle scores. All agree that after 2-5 years, patients who sustain a pilon fracture still have significantly poorer general health scores than the average population. 15-30% were disabled and 40% had changed jobs as a result of the fracture. OA was present in 50% or more patients, usually within 2 years, but clinical outcome correlated poorly with OA severity. The overall rate of fusion for post-traumatic OA was about 10%. Marsh found that patients continued to improve for up to 5 years after a pilon fracture and this should be borne in mind when assessing results from shorter follow-up. The main predictors of final outcome were the severity of the original injury (in all series) and the quality of the initial reduction.
Volgas (2010) looked at the effect of a pilon fracture on patients' ability to cope in work and financially (in the US setting). All 3 white-collar workers returned to work at 1 year but only 3/21 blue-collar workers did so. 5/8 college graduates returned to work compared with 2/14 non-graduates. 42% of patients used social assistance and 37% had to sell possessions to meet financial obligations.
