What is it?
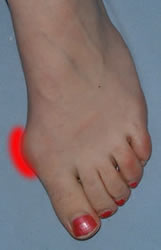
- Lateral deviation of the great toe at the metatarsophalangeal (MTP) joint.
- The metatarsal head is deviated medially so there is pressure on the medial side of the metatarsal head which may produce a bursa (bunion), or even skin breakdown or infection.
What do people complain of?
- Pain, swelling, shoe pressure or skin breakdown over the medial side of the 1 st metatarsal head
- Pain in the 1 st MTP joint
- Neuritic pain, numbness or tingling down the toe
- Difficulty in getting shoes to fit, sometimes under pressure from work dress codes or safety rules
- Concern that the toe may become symptomatic or untreatable in the future (“should something be done before I end up like my mother?”)
- Dislike of the appearance of the foot
Things to think about
- What is the patient actually complaining of? Can that be improved?
- Where are the pain and the bump? If they are on the dorsum of the MTP joint rather than the medial side, it’s more likely the main problem is OA (hallux rigidus)
- Could they have an underlying condition like rheumatoid arthritis or a hypermobility syndrome?
- Is this a high-risk problem – diabetes, peripheral vascular disease, neuropathy, infection?
Principles of treatment
- Explanation and simple advice are most important.
- Make the shoe fit the foot, not the foot fit the shoe. Advice on finding shoes of reasonable design, and safety shoes with extra room can be arranged by the orthotists. Unwillingness to wear shoes that fit is not a indication for surgery. The primary goal of treatment is comfort not cosmesis.
- Pain in the joint can usually be managed with appropriate footwear and simple analgesics. If this does not work the MSK podiatrist can advise on whether an orthotic device may be helpful.
- There is no evidence that corrective splints or orthoses change the deformity or level of pain, and they are not recommended
- A history of skin breakdown, infection or underlying disease increases both the risks of further serious problems and the risk of surgery, but may tip the balance towards surgery to minimise long-term risk. We would view recurrent skin breakdown or infection as an indication for early review, at lest in MSK.
- Symptoms of nerve irritation do not reliably recover after correction, although they may tip the balance in favour of surgery.
- There is no evidence that early intervention to prevent deterioration is effective, rather than reserving treatment until there is a problem that warrants it. Early intervention would, however, expose minimally symptomatic people to the standard risks of surgery.
- We do not offer surgery simply to improve the appearance of the foot.
- If simple treatment, including appropriate shoewear, fails and the patient understands the risks and realistic outcomes of surgery, a metatarsal osteotomy is usually the most appropriate corrective technique. Most studies report 80-90% patient satisfaction, and there is little evidence that any procedure is any better than another. We favour methods that allow day-case surgery and early weightbearing mobilisation. Bilateral surgery and other simultaneous procedures (lesser toe straightening, bunionette correction, neuroma excision etc) are practical for most but not all patients. We quote a serious complication rate of about 5%.
