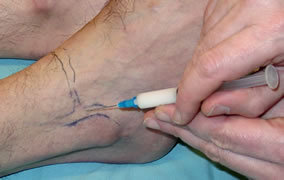
Injection can be diagnostic and therapeutic
Debridement of synovitis and an anterior tibial spur
Non-surgical management
Most patients will get some benefit from local physiotherapy and an ankle rehabilitation programme to address instability and synovitis. Some struggle to complete the programme, however, due to pain on loading the ankle, and may benefit from a steroid injection before continuing. There is little information on the effectiveness of such nonsurgical treatment.
Surgery
Patients with persistent disabling pain may be offered an arthroscopic debridement. Even in the presence of mechanical instability, synovial debridement is often effective in relieving symptoms and stabilisation may not be required (Laing 2004). Usually the synovitis and adhesions are found mainly in the anterolateral joint, often with synovitis descending from the inferior tibiofibular joint. Spurs can be debrided with a burr. It is important to inspect the joint surface carefully; at least 10% have an unsuspected chondral or osteochondral lesion which can be debrided. We encourage active range of movement exercises and weightbearing as soon after surgery as possible.
At 5-8y after arthroscopic debridement, Tol (2001) reported satisfactory results in all patients without osteoarthritic changes. 77% of patients with grade-1 OA and half of those with grade-2 OA got good results. Hassouna (2007) reviewed 80 patients at a mean 4yr after anterior debridement. 55 had soft tissue impingement or spurs only, while 25 had moderate to severe osteoarthritis. 14/25 in the OA group had an ankle fusion in the folllow-up period and 6 had repeat arthroscopies. None of the non-arthritic group had further surgery. Rasmussen found 62% of patients to be pain-free at 2y irrespective of pathology, while 27% had a useful improvement in pain.
Scranton and McDermott (1992) found that patients recovered more quickly after arthroscopic than open debridement. However, Coull et al (2003) reported excellent results with open debridement – 92% of patients had little or no pain or activity limitation at 5-9y provided they had normal joint space pre-operatively.
Most spurs reform (Tol 2001), but recurrent symptoms are not common, and published series do not report re-operations for recurrent spurs. Similarly, in the series referred to, spurs did not progress to arthritis, and early arthritis did not progress.
