Aetiology
The development of hallux valgus appears to depend partly on genetic factors and partly on environment, especially shoewear. The genetic effect may be partly related to hypermobility. Any specific condition which reduces the stability of the 1st MTP joint (and other first ray joints) also increases the risk of hallux valgus:
- Inflammatory arthritis such as rheumatoid disease, psoriatic arthritis or Reiter’s syndrome
- Hypermobility syndromes such as Ehlers-Danlos syndrome, Down’s syndrome or Marfan’s syndrome
- Muscle imbalance in the foot due to cerebral palsy, myelomeningocoele or stroke may produce a hallux valgus deformity. Hallux valgus is uncommon in the muscle imbalances which produce pes cavus, probably because the plantar-flexed first ray is more difficult to deform in the transverse plane.
Pathogenesis
How does the deformity actually develop? In particular, which comes first, valgus deviation of the phalanx or metatarsus primus varus?
Truslow wrote a paper in 1926 which argued that metatarsus primus varus was the initial abnormality, with the phalanx collapsing into the gap between first and second rays. His paper actually produced no evidence to support his hypotheses. However, Kilmartin studied schoolchildren’s feet and found that some children with hallux valgus and metatarsus primus varus on one foot, but only metatarsus primus varus on the other. He argued that, as hallux valgus is often bilateral, isolated metatarsus primus varus was the predisposing factor for hallux valgus in at least some feet.
On the other hand, Hardy and Clapham studied the hallux valgus (HVA) and intermetatarsal (IMA) angles in a large group of schoolchildren and found that, on average, increase in HVA predated increase in IMA by about a year. Antrobus noted that correcting the HVA leads to subsequent reduction in the IMA, implying that the deviated phalanx is at least one of the driving factors for metatarsal angulation. Similar results have been reported after Keller and fusion procedures.
It seems that phalangeal angulation is probably the initial deformity, at least in most people. However, by the time of clinical presentation, first metatarsal varus is sufficiently fixed that it will not entirely resolve spontaneously if the phalanx is realigned. Therefore, surgical correction normally requires a first metatarsal osteotomy. In mild deformities, there may be a role for pure soft tissue correction.
Shoes are generally implicated as the main force driving the phalangeal deformity. However, Root and others have emphasised the effect of ground reaction force on the medial side of the first ray in people with overpronated feet, usually associated with subtalar valgus. Tanaka et al (1999) found that mean subtalar valgus was higher in patients with hallux valgus than in normal controls. Komeda (2001) found the talus to be more plantarflexed and the navicular lower in hallux valgus feet than controls. However, no study has yet shown that correction of hindfoot valgus or arch lowering can prevent hallux valgus from developing or recurring after surgery.
First ray instability - chicken or egg?
There has been considerable research interest in the possibility that instability of the first metatarsal, particularly at the tarsometatarsal joint, leads to hallux valgus. This was proposed by Courriades and promoted by Lapidus, who fused the first TMT joint, along with a distal soft tissue correction, to correct hallux valgus (Lapidus procedure).
A number of studies (Wanivenhaus 1989, Klaue 1994, Faber 1999) have used various methods to quantify first ray stability in the vertical plane, most of which have shown greater first ray mobility in patients with hallux valgus than in the general population. Not all of these papers have determined the errors of their measurement techniques, and none have shown that vertical mobility of the first TMT joint correlates with transverse mobility, which would be necessary to produce metatarsus primus varus.
A couple of the papers do recognise that association does not prove causality, and that it might even be that hallux valgus causes instability, rather than instability causing hallux valgus.
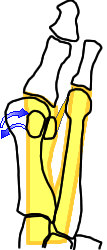
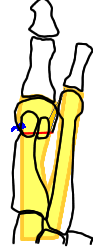
Outside the plantar fascia envelope (L) the first metatarsal is more mobile. Brought back within the plantar fascia(R) the mobility decreases. It is not necessary to fuse the TMT joint (Lapidus procedure) to achieve this.
Recent work suggests that this might, indeed, be the case! Rush (2000) showed that the first metatarsal is stable in the normal position, loses this stability if positioned in varus, and regains much of its stability if repositioned in correct alignment by metatarsal osteotomy. Coughlin (2004) showed that first metatarsal mobility was decreased in ankle dorsiflexion (when the plantar fascia is tighter) and increased by a functioning plantar fascial windlass mechanism. The available evidence suggest this is because the first ray comes back under the control of the plantar fascia when it is repositioned in line.
Clinical studies tend to support these recent findings. Mann showed that failure of correction of hallux valgus was not associated with first metatarsal instability. More convincingly, Faber et al (2004) reported a study in which 87 patients, about half of whom had instability according to a recognised method, were randomised to a Lapidus procedure or a distal metatarsal osteotomy. There were no difference in clinical outcome even in the unstable groups. Coughlin (2007) and Kim (2008) both showed that first metatarsal mobility was decreased after a Mann procedure for hallux valgus. Coughlin found that 23/122 feet had >9mm mobility pre-op compared with 2/122 post-op, and mean mobility diminished from 7.2mm to 4.5mm. In Kim's study mean mobility was reduced from 6.8 to 3.2mm, and the improvement was greater in the hypermobile group. Smith (2008) reviewed this evidence helpfully.
It appears that first metatarsal instability is not very important in the causation of hallux valgus or in determining the outcome of treatment. Most likely it is a manifestation of the loss of plantar fascial control over the first ray when the first metatarsal and proximal phalanx are not correctly aligned, and can be corrected by the procedure which would be advised for that patient if hypermobility was not present.
