General examination
A quick but systematic general examination will put the patient's symptoms in context. Check for evidence of:
- generalised inflammatory arthropathy
- peripheral neuropathy, eg in diabetes, using Semmes-Weinstein neurofilaments
- significant peripheral vascular disease, obtaining ankle-brachial index if necessary
- neurological imbalance
- hypermobility syndromes
- proximal defomity or limb length discrepancy relevant to the presenting symptoms
Examination of the foot
Examnine the whole foot, looking at the overall shape. Hallux valgus is commoner in flat or neutral feet. Metatarsus adductus makes it more difficult to correct hallux valgus.
Look for deformities such as flatfoot or deforming forces such as tightness of the gastrocnemius/soleus which might contribute to recurrence of deformity or make correction more challenging.
Examine the hallux and the rest of the forefoot.
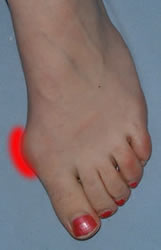
Measure the severity of the deformity (including any pronation of the great toe) Assess the size of the medial eminence and the state of the overlying skin, especially any evidence of infection
Try to correct the MTP joint deformity, then manipulate the toe in the corrected position to check range of movement and whether movement and axial compression (the grind test) cause pain - usually due to arthritis
In this case the MTP joint will not correct passively.
Causes include
- soft tissue contracture
- congruent joint
- MTPJ arthritis
For exams, test mobility of the first metatarsal. Although this is increased, on average, in patients with hallux valgus, it now seems that this is most likely due to the hallux vagus deformity, will reduce with deformity correction, and does not need treating in any special way.
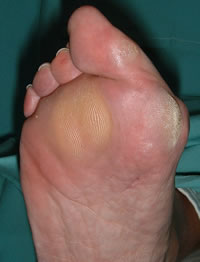
Look for calluses:
- under the medial border of the hallux, often in a pronated toe
- under the lesser metatarsal heads
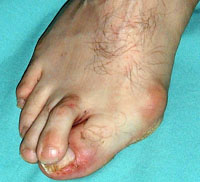
Look for associated lesser toe problems, such as an over-riding second toe
