Focusing the clinical assessment
Based on the biomechanical model, we would want to be able to differentiate between stable and unstable fractures. All displaced fractures, by definition, are unstable, but there could be a group of undisplaced fractures which are unstable and might need more active treatment. Among more severe injuries, we also want to identify dislocations, particularly those at risk of skin breakdown, patients with major damage to the soft tissue envelope as shown by severe swelling and blistering, and, of course, open fractures. As with all fractures, we need to identify nerve and vascular injuries and compartment syndrome, all of which are fortunately rare.
We need to identify relevant patient factors that might determine desired or achievable outcome: oc- cupation, sports, previous mobility; and co-morbidities, especially those such as diabetes, vascular disease and skin problems, which increase treatment risks.
Most of these can be identified by a focused history and examination.
History
Patients with ankle fractures normally give a history of a fall or other injury mechanism. Absence of injury should make one consider a neuropathic fracture. Some patients hear a crack which is usually in favour of a major ligament injury or fracture. Other indications of the severity of injury include whether the patient was able to stand on the ankle, to walk, run, continue sport or other activity after injury.
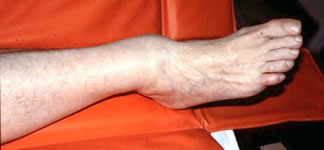
The obvious deformity risks medial skin necrosis. This ankle needs immediate provisional reduction
Examination
A general survey of the patient should be undertaken, as meticulous as indicated by the history and severity of injury. There may be obvious malalignment of the ankle. If this is imperilling the skin over the medial side, the ankle needs to be reduced urgently. Inspect the skin and subcutaneous tissues for open fractures, fracture blisters and swelling.
Palpation of the acutely injured ankle should begin at the proximal fibula. The length of the fibula is palpated for tenderness, swelling or disruption to the bony contour, along with the tibiofibular interosseous area, especially the inferior tibiofibular joint. Clinical evidence of a malleolar fracture should be sought by palpation. If in doubt, stressing the malleoli by pushing the talus medially or externally rotating it may produce pain or displacement, but this is unnecessarily painful if there is already strong evidence of fracture. In undisplaced fractures, carefully examine the soft tissue of the medial side. Tenderness, swelling and bruising here are suggestive of a tear of the deltoid ligament and hence of potential instability. The calcaneum, midfoot and 5th metatarsal should also be examined.
Check the sensation, circulation and pulses. Examine the Achilles, long flexor and peroneal tendons.
Clinical findings can then be used according to the Ottawa Ankle Rule to decide whether radiographs are necessary
