There are two key questions in treatment planning for a patient with a fractured ankle:
- is it displaced?
- if not, is it stable?
Is it displaced?
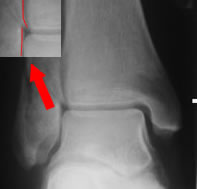
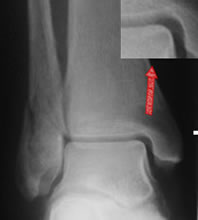
"Displacement" refers to the position of the talus in the mortise (left), not the malleolar fragments (right)
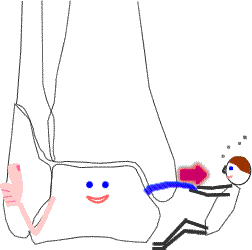
An intact deep deltoid will keep the talus safe in the mortise
What counts as displacement?
Displacement refers to the position of the talus in the mortise, NOT minor displacements of the fibula. The discussion of the basic science of ankle stability showed why fibular displacement in itself is of little significance:
- an intact deep deltoid ligament will keep the talus in the mortise in the face of fibular displacement
- apparent fibular displacements do not normally represent mortise incongruity
Must the talus be exactly congruent?
Several older papers recommended no more than 4mm medial clear space (MCS), or 2mm more than the superior clear space. Recent studies suggest 5mm MCS is compatible with an intact deep deltoid ligament. None of these measurements were made on standing films, which may be a more accurate assessment of congruity.
Is it stable?
Stability can be defined in different ways. Ideally, a stable fracture would be one that can be treated without splintage, with early rehabilitation and with minimal incovenience to the patient. In some literature "stable" seems to have the less ambitious meaning of "does not need internal fixation", although this might be more a statement about orthopaedic culture than about fracture biology! Often stability has been defined in terms of the result of tests - and this can, obviously, be useful - but care needs to be taken that the test result can be shown to make a difference for management. The work on stress testing is open to this critique.
Previous work
Until recently, most studies have proceeded as though "stable fractures" or "supination-external rotation stage 2 fractures" are self-apparent, or can be defined in terms of:
- undisplaced, isolated, lateral malleolus fracture. Fox (2005) explicitly discounted fractures above the syndesmosis
- no medial tenderness, bruising or swelling
- Fox also required a low-energy fracture with an intact soft tissue envelope
Stress radiography
In 2004 McConnell and then Egol reported the results of stress radiography of undisplaced lateral malleolar fractures, with markedly different results. Both used >4mm MCS as a positive stress test. 63% of McConnell's patients had a negative stress test compared with only 35% of Egol's. Both series reported that physical sign were only moderately predictive of the result of the stress test. In Egol's series, 30% had a positive stress test but no medial symptoms or signs. 20 of these patients were treated in ankle braces and two displaced, although only one was symptomatic. Patients in McConnell's series with negative tests were treated in ankle braces and all united uneventfully.
The above studies used a manually applied external rotation stress test. An alternative technique is the gravity stress test, originally described by Michelson. The patient lies in the lateral position and the ankle is allowed to hang down freely over a support. Schock et al (2006) reported that this was less uncomfortable and possibly more sensitive than the manual stress test. 50% had an abnormal stress test, although no additional imging or clinical results were reported.
Weber (2010) reported 56 patients with undisplaced lateral malleolar fractures. Medial symptoms and signs were not reported. The patients were initially splinted with partial weight bearing, and had unprotected standing mortise/lateral Xrays at 3-10 days post fracture. 5/56 (9%) displaced and were fixed. The others had a variety of splintage. There was no late subluxation, two delayed unions and two patients developed chronic pain syndromes. Mean AOFAS score was 96.1/100. Weber commented that “…relevant instability is largely overestimated by the stress manual or gravity stress radiographs.”
Imaging the deep deltoid
Egol and Koval have moved on to investigate the significance of positive stress radiographs with MR imaging of the deep deltoid ligament. Their most recent report found that 91% of patient with positive stress radiographs had only partial deltoid tears and successfully treated in a walking boot. Overall, this would suggest an incidence of complete tears of 6% (0.09x0.65).
At the same meeting (OTA 2006), Zeni reported ultrasonography of the deep deltoid ligament in patients with undisplaced ankle fractures. Fourteen patients had norml ligaments, 8 had partial tears and 5(18.5%) had complete tears. Physical signs were moderately predictive of any tear, but the absence of medial signs was 100% predictive of the absence of a complete tear.
Pragmatic treatment
Fox et al (2005) took a different, more pragmatic, approach. Stable fractures were diagnosed on the basis of medial symptoms and signs. 63% of undisplaced fractures fell into this category, and were successfully treated in ankle braces. The remainder, mainly on the basis of medial signs but a few on fracture morphology, were viewed as potentially unstable and were treated in BKW casts. Two fractures (1% of undisplaced fractures, 2% potentially unstable fractures) displaced. Akhtar (2009) described the potentially unstable fractures in more detail and with larger numbers. Over 10 years, 153 potentially unstable fractures were treated in BKW casts, with a standing Xray at one week. Unlike Weber's series, the one-week weightbearing image was taken in cast. 3/153 (2%) fractures displaced, all in the first week. This supports the view that even potentially unstable fractures are usually, in practice, stable.
This issue has been discussed in some detail because
- it is crucial to modernising the management of ankle fractures
- it is once again an area of active study where conclusions may have to be modified further
Recommendations
Currently, our assessment of the evidence on displacement and stability is:
- displacement is to be judged on talar position in the mortise, not fragment position
- either 4mm or 5mm of medial clear space would be justifiable as a starting point to define displacement, but 5mm is attracting incresing supporting evidence
- medial signs are probably adequate to identify important deep deltoid injuries
- stress radiography probably overestimates the prevalence of important deep deltoid injuries
- the prevalence of important deep deltoid injuries seems to lie between 1-20% of undisplaced fractures - as the highest estimate was in much the smallest study, the true value is probably in the lower part of this range.
- if stress radiography is felt necessary, the gravity stress test may be more acceptable to patients than manual testing
